The evolution of risk-shifting between payers, patients, and manufacturers is not completely accounted for in the structuring of rebate contracts. Much of the focus of these negotiations center around relative copay differentials and utilization management restrictions. Often ignored is the fact that, for many drugs, patients seldom pay the negotiated copay amounts. The rise of medical and pharmacy deductibles that total thousands of dollars negate these negotiated copays. These deductibles also call into question who is the beneficiary of these rebates.
Consider, for example, a drug with a $5,000 annual cost for a patient with a $4,000 annual insurance deductible. There is a possibility that some amount of this deductible, up to a maximum of $4,000, could result in a patient paying full price for the drug for a substantial portion of the year before any cost sharing is activated. Percentage rebates paid by a manufacturer under this scenario result in payers receiving funds for a drug that the patient has actually paid the bill for.
We looked across the HealthPlanView database and calculated the average deductible for the leading payers, weighting this average based on insured lives attributable to specific plan designs, for 2019 Commercial Insurance Benefit Designs. Here’s what we found.
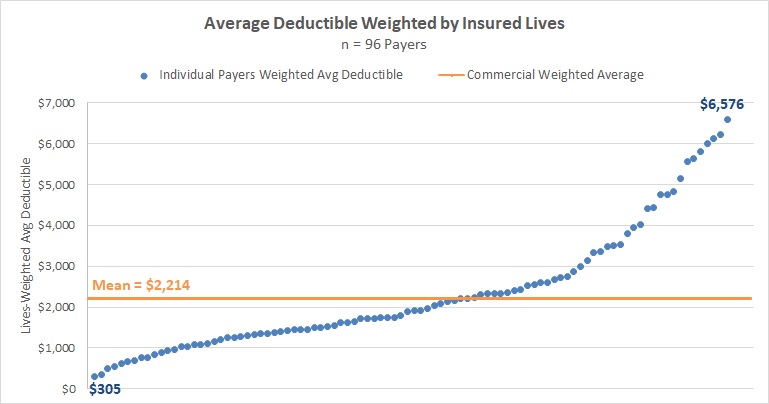
With a mean lives-weighted average deductible of $2,214 and over 20% of all commercial enrollment in plans with deductibles above $4,000, it is clear that the value of a copay to a patient varies widely. Depending on the annual cost incurred by the patient, many patients may be taking on more financial risk for drug cost than the insurers whom they pay for coverage. The HealthPlanView web tool helps clients understand this dynamic by isolating drug cost for each benefit design and attributable insured lives for each payer, allowing users to weigh the true impact of paying for preferred access.
If you are interested to learn more about HealthPlanView, contact Nicole Espinoza, VP, Knowledge Management at Nicole.Espinoza@pharmspective.com.
